Anaesthesia technology refers to medical systems that support safe, pain-controlled procedures. It combines machine software and drug monitoring tools, ensuring patient comfort. Modern anaesthesia technology improves surgical precision, safety recovery outcomes worldwide. Healthcare facilities rely on anaesthesia technology for consistent, reliable procedural support. This technology integrates engineering, medicine, pharmacology, and digital monitoring advancements.
Historically, anaesthesia involved basic methods with limited patient safety controls. Technological progress transformed anaesthesia into a precise data data-driven medical field. Modern systems allow controlled sedation, unconsciousness, and pain management accurately. Technology reduced surgical risks, improved outcomes, and expanded complex procedure possibilities. Understanding anaesthesia technology helps appreciate its critical healthcare role.
Anaesthesia technology supports surgeons, anesthesiologists nurses throughout medical procedures. It ensures stable vital functions while procedures occur without patient awareness. Advanced monitoring alerts clinicians to physiological changes instantly. Technology enhances decision-making through real-time patient data analysis. This field continues evolving alongside digital healthcare innovations.
Table of Contents
Core Components of Anaesthesia Tech
Anaesthesia technology includes machines delivering controlled anesthetic gas mixtures safely. These machines regulate oxygen and anesthetic concentration, airflow pressure precisely. Integrated safety systems prevent hypoxia, overdosing equipment malfunction events. Modern machines include digital displays, alarms, and automated controls. They support consistent delivery across varied surgical environments.
Vaporizers convert liquid anesthetics into controlled inhalable gas forms. Ventilators assist breathing when patients cannot breathe independently. Flow meters control gas volumes delivered during anaesthesia administration. Filters and circuits maintain cleanliness, temperature, and humidity levels. Each component ensures stable patient respiratory support.
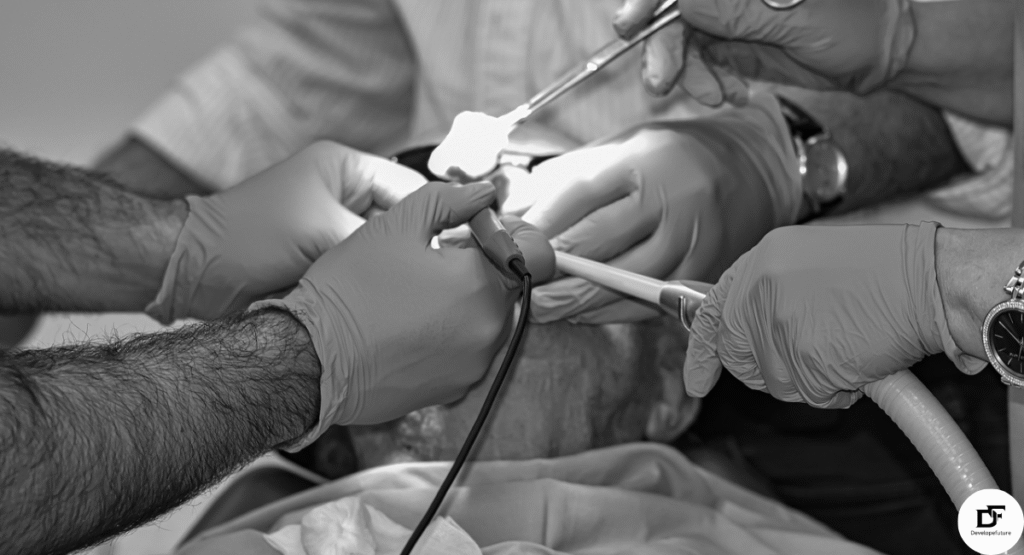
Role of Monitoring Systems in Anaesthesia
Monitoring systems track vital signs during anaesthesia continuously. They measure heart rate, blood pressure, oxygen saturation respiration. Real-time monitoring enables rapid detection of dangerous physiological changes. Alarms notify clinicians immediately when parameters exceed safe limits. This constant surveillance significantly reduces anaesthesia-related complications.
Advanced monitors include capnography, electrocardiography temperature monitoring systems. Capnography measures carbon dioxide levels reflecting ventilation effectiveness. Electrocardiography tracks cardiac rhythm, detecting arrhythmias early. Temperature monitoring prevents hypothermia during long surgical procedures. Together, these systems support comprehensive patient safety.
Types of Anaesthesia Supported by Tech
Anaesthesia technology supports general, regional, and sedation techniques. General anaesthesia induces unconsciousness with complete pain sensation. Technology precisely controls the depth and duration of unconsciousness. Ventilation systems maintain breathing during unconscious states. Monitoring ensures patient stability throughout procedures.
Regional anaesthesia numbs specific body areas using nerve blocks. Technology assists accurate drug delivery using imaging guidance. Local anaesthesia targets small areas for minor procedures. Sedation technology manages anxiety while maintaining patient responsiveness. Each type benefits from technological precision.
Digital Advancements in Anaesthesia Equipment
Digital interfaces improved usability, accuracy, and workflow efficiency. Touchscreen displays present vital data clearly for clinicians. Software algorithms assist dosage calculations, reducing human error risks. Electronic records integrate anaesthesia data into patient histories. This improves continuity of care across departments.
Automation allows controlled drug delivery through infusion pumps. Smart pumps adjust dosages based on patient responses. Decision support systems analyze trends and suggest interventions. Digital connectivity enables remote monitoring and expert consultation. These advancements enhance safety and efficiency.
Safety Features in Modern Anaesthesia Tech
Modern anaesthesia technology prioritizes multiple safety redundancies. Built-in alarms detect pressure flow oxygen concentration abnormalities. Fail-safe mechanisms activate backup oxygen during system failures. Self-testing routines identify equipment faults before procedures. These features reduce preventable anaesthesia accidents.
Color coding standardization prevents incorrect gas connections. Lockout systems avoid incompatible component misuse errors. Data logs support incident review and quality improvement. Regular software updates maintain safety compliance standards. Safety design protects both patients and clinicians.
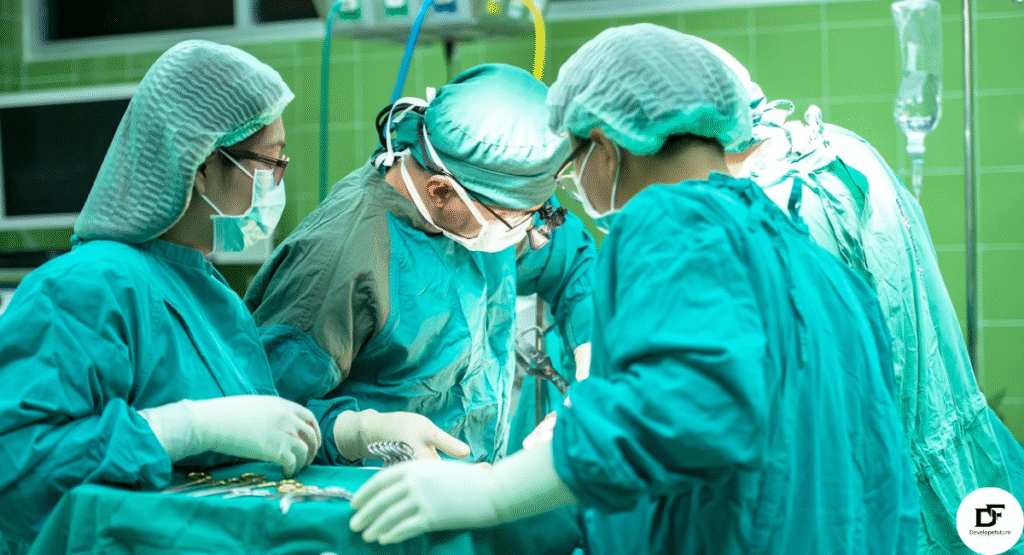
Anaesthesia Tech in Surgical Environments
Operating rooms rely heavily on integrated anaesthesia systems. These systems coordinate with surgical lighting and imaging equipment. Space-efficient designs support workflow without clutter interference. Mobile units allow flexible placement across operating theaters. Integration improves surgical team coordination.
Anaesthesia workstations centralize controls, monitoring, and documentation. Ergonomic layouts reduce clinician fatigue during long surgeries. Network connectivity shares data with hospital information systems. This integration supports efficiency and accurate record-keeping. Surgical outcomes benefit from seamless technology coordination.
Training and Skill Requirements for Anaesthesia Tech
Operating anaesthesia technology requires specialized professional training. Anesthesiologists and technologists learn equipment operation and troubleshooting skills. Simulation-based training improves response to emergency scenarios. Continuous education ensures familiarity with evolving technologies. Proper training maximizes technology effectiveness and patient safety.
Technicians maintain, calibrate, and repair anaesthesia equipment regularly. Understanding software and hardware interactions is increasingly important. Interdisciplinary teamwork supports optimal technology utilization. Competency standards ensure consistent safe practice across facilities. Education remains essential for advancing anaesthesia care.
Maintenance and Quality Control of Anaesthesia Equipment
Regular maintenance ensures anaesthesia technology performs reliably. Scheduled inspections identify wear, leaks calibration issues early. Preventive maintenance reduces unexpected equipment failures during surgeries. Documentation tracks service history and compliance requirements. Quality control protects patient safety standards.
Biomedical engineers oversee testing, validation, and certification processes. Sterilization protocols prevent infection transmission risks. Software updates address bugs, security vulnerabilities improvements. Equipment lifecycle management supports timely replacement planning. Maintenance programs sustain long-term technology reliability.
Future Trends in Anaesthesia Technology
Future anaesthesia technology emphasizes personalization through data analytics. Artificial intelligence may predict patient responses to anesthetics. Closed-loop systems automatically adjust drug delivery precisely. Wearable sensors could extend monitoring beyond operating rooms. Innovation aims to further reduce risks.
Tele anaesthesia may support remote expert guidance during procedures. Cloud platforms enable centralized data analysis across hospitals. Sustainability drives the development of energy-efficient equipment designs. Patient-centered technology enhances comfort recovery experiences. The future promises safer, smarter anaesthesia care.
FAQ’s
What is anaesthesia technology used for in healthcare?
Anaesthesia technology supports pain control, sedation monitoring during medical procedures. It ensures patient comfort, unconsciousness, and physiological stability. Technology allows precise control over anesthetic delivery. Monitoring systems detect risks early during surgeries. It enables safe complex medical interventions.
Who operates anesthesia technology during surgeries?
Anesthesiologists primarily operate anaesthesia technology during procedures. They work alongside trained anaesthesia technologists and nurses. Teams monitor patient responses and adjust settings continuously. Proper training ensures safe technology use. Collaboration ensures optimal patient outcomes.
How does anaesthesia technology improve patient safety?
Technology provides continuous real-time monitoring of vital signs. Alarms alert clinicians to dangerous physiological changes immediately. Precision dosing reduces medication-related risks. Safety redundancies prevent equipment failure consequences. Risk reduction improves surgical safety.
Is anaesthesia technology used outside operating rooms?
Anaesthesia technology is used in diagnostic and emergency settings. It supports procedures like endoscopy imaging interventions. Portable systems enable use in intensive care units. Sedation technology assists minor outpatient procedures. Its applications extend beyond surgery.
What skills are required to manage anaesthesia technology?
Professionals need technical knowledge, clinical judgment equipment familiarity. Training includes emergency response practice. Understanding monitoring data interpretation is essential. Continuous education keeps skills current. Competence ensures safe, effective anaesthesia care.
Conclusion
Anaesthesia technology is essential for modern, safe surgical care. It integrates machine monitoring, drugs, and digital intelligence. Technology transformed anaesthesia into a precise, controlled medical discipline. Continuous innovation improves outcomes and reduces risks worldwide. Understanding this technology highlights its healthcare importance.
As medicine advances, anaesthesia technology will continue evolving rapidly. Training, maintenance, and safety remain critical success factors. Digital integration will enhance efficiency, accuracy, and patient experiences. Future developments promise even greater safety personalization benefits. Anaesthesia technology remains foundational to modern surgery.




